Last Tuesday, a care manager in Manchester spent four hours reviewing her team’s compliance folders, only to realize her staff were still referencing outdated 2012 protocols rather than the 2022 standards. It’s a stressful reality for many leaders who prioritize person-centered care but feel buried by administrative shifts. Understanding the nuances of the social care and health act framework is essential for protecting the independence of your residents and the reputation of your service. We know you want to focus on the warmth of human connection, not the cold text of a legal document.
You likely feel that the constant stream of legislative updates from Whitehall makes it difficult to maintain a "calm in the storm" environment for your families. We’ve created this guide to translate complex law into actionable daily policies that ensure peace of mind for everyone involved. We promise to break down the 2022 reforms and the 2026 outlook without the confusing jargon that often clutters official handbooks.
This guide provides a clear timeline of UK care legislation and practical steps to ensure your next CQC inspection is met with confidence. You’ll learn how to align your bespoke care plans with current legal requirements while keeping your team’s focus on the dignity of every individual you serve.
Key Takeaways
-
You will understand the evolution of UK legislation, helping you transition smoothly from older frameworks to the modern requirements of the 2022 Health and Care Act.
-
We show you how to navigate the social care and health act with confidence, ensuring your daily operations meet the latest compliance standards while protecting your clients’ independence.
-
Learn how to bridge the gap between health and care services through Integrated Care Systems, creating a more seamless and supportive journey for the families you serve.
-
Discover practical ways to align your service with the CQC’s Single Assessment Framework, ensuring you remain "Well-led" and "Effective" under the 2026 benchmarks.
-
Explore how adopting a bespoke digital roadmap can future-proof your care service, providing the peace of mind that comes with streamlined, modern management.
Table of Contents
Understanding the UK Social Care and Health Legislative Landscape
Understanding the legal framework behind your care shouldn’t feel like a chore. We believe that clarity brings peace of mind when you’re making big decisions for your family. The primary social care and health act legislation in the UK exists to ensure that every individual receives support that respects their dignity and independence. These laws aren’t just dry documents; they’re the safeguards that guarantee your right to person-centred support. By 2026, the Department of Health and Social Care (DHSC) will continue to refine these standards, focusing on a more joined-up approach to funding and delivery that prioritizes the quality of life for every family across the country.
Legislation exists because everyone deserves to feel safe and respected in their own home. It moves the focus away from institutional tasks and toward the human being at the centre of the service. We see these acts as a promise of compassion. They ensure that your care is a collaborative, respectful process rather than a mere transaction. This legal backbone gives you the power to demand high standards and the security of knowing that those standards are backed by the weight of the law.
The Legal Pillars: 2008, 2012, and 2022
The Health and Social Care Act 2008 was a landmark moment that established the Care Quality Commission (CQC). It gave us a watchful eye to ensure safety across all providers, from hospitals to home-based support. This was followed by the Health and Social Care Act 2012, which famously introduced the principle of "no decision about me, without me." It shifted the power back to you. Most recently, the 2022 Health and Care Act arrived on 1 July 2022, creating 42 Integrated Care Boards (ICBs) across England. This change aims to remove the barriers between your GP, the hospital, and your local care services.
Who These Acts Protect
These laws protect your right to bespoke care. You deserve a plan that fits your life, not a one-size-fits-all service. Legislation also supports our dedicated professionals by setting clear legal standards for training and conduct. It ensures "continuity of care," meaning if a provider changes, your support shouldn’t just stop. We know how vital that stability is for your family’s routine. The social care and health act framework ensures that whether you’re at home or in a clinical setting, your voice remains the most important one in the room.
-
Service Users: Guaranteed rights to dignity, privacy, and personalized care plans.
-
Families: Peace of mind through regulated standards and clear pathways for feedback.
-
Care Staff: Clear professional boundaries and mandatory training requirements to ensure safety.
-
Providers: A structured environment that rewards high-quality, compassionate service.
The Health and Social Care Act 2012: A Turning Point
The 2012 social care and health act reshaped how we think about support in the UK by introducing the most significant restructure of the NHS since its inception. By establishing Clinical Commissioning Groups (CCGs), the government placed approximately 80% of the NHS budget directly into the hands of GPs and clinicians. This shift aimed to ensure that those closest to patients were making the decisions about their care. Local authorities also took on new, statutory duties for public health, creating a more integrated approach to community wellbeing. You can read the full legal framework in the original Health and Social Care Act 2012 to see how these duties were codified.
This legislation also prioritised your voice through the creation of Healthwatch England. This body acts as a national champion for users of health and social care services, ensuring that your feedback leads to real change. Transparency became a legal cornerstone with the introduction of the statutory Duty of Candour. This requires care providers to be open and honest with families when something goes wrong, fostering a culture of trust rather than one of blame. To manage these complex requirements, many providers transitioned to digital care management software UK , which allows for real-time updates and clear communication between staff and families.
The Rise of Personalisation
The 2012 Act moved the sector away from rigid, institutional routines toward a model of "choice and control." We now see this in how domiciliary and residential settings build support around the individual’s lifestyle rather than the facility’s schedule. Personalised Care is a statutory requirement that ensures every individual’s specific needs and preferences dictate their support plan, moving beyond a standard one-size-fits-all approach. This shift empowers you to decide how, when, and where you receive support, preserving your dignity and independence at home.
Oversight and Regulation
Regulation became much more rigorous following the 2012 reforms. The Care Quality Commission (CQC) received strengthened enforcement powers to ensure every provider meets high safety standards. This legal framework makes it vital for providers to maintain cqc compliant care policies and procedures at all times. Accuracy is no longer optional; the legal necessity of precise incident and accident reporting ensures that every event is analysed to prevent future risks. Our team can help you understand how these regulations protect your loved ones through our bespoke support options tailored to your family’s needs.
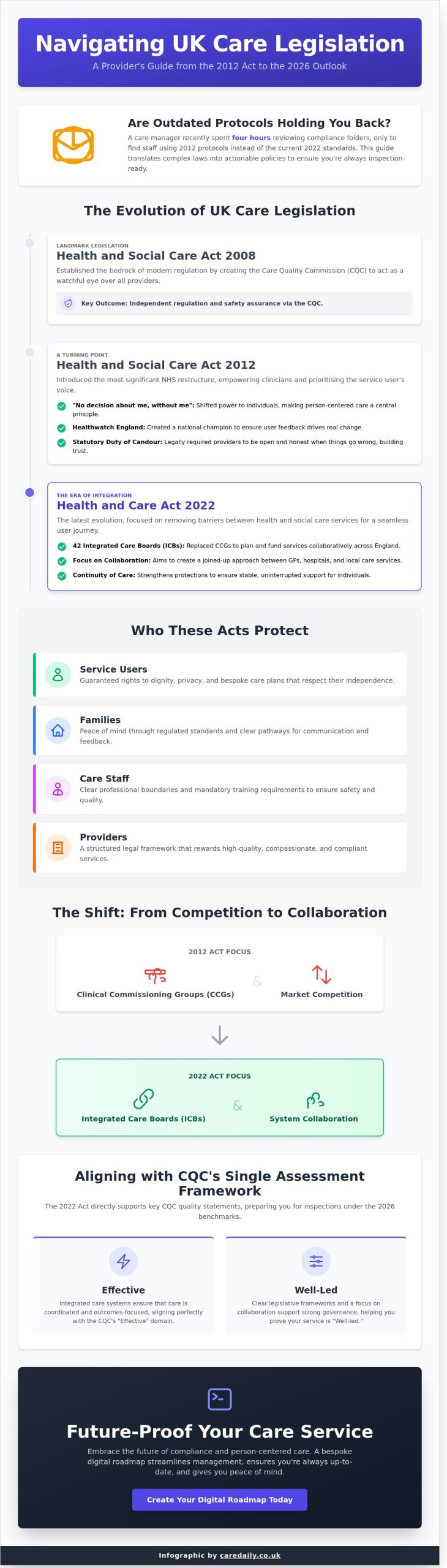
The Health and Care Act 2022: The Era of Integration
For years, the wall between hospital services and home-based support felt too high. Families often found themselves repeating their stories to different professionals, from GPs to social workers. The Health and Care Act 2022 was designed to tear down these silos. It focuses on a simple idea: care should revolve around you, not the system’s internal boundaries. By making Integrated Care Systems (ICS) legal entities on 1 July 2022, the government moved away from internal competition. This social care and health act creates a framework where doctors, social workers, and local charities work as a single team to support your dignity and independence.
Joining Up the System
We know that leaving the hospital can be a stressful time for your family. The 2022 Act introduces Integrated Care Boards (ICBs) to oversee local NHS budgets and planning. These boards have a legal duty to cooperate with local authorities. This change directly improves "step-down" care services. Instead of waiting in a hospital bed because a care package isn’t ready, the new system encourages faster, safer discharges. By 2026, the goal is for every local area to have a seamless pathway that supports your life at home. It’s about ensuring you get the right support at the right time, providing peace of mind for everyone involved.
The Digital Mandate
Paper files are becoming a thing of the past. The legislation introduces a mandate for the Digital Social Care Record (DSCR). The Department of Health and Social Care set a target for 80% of CQC-registered providers to adopt digital records by March 2024. This isn’t just about technology; it’s about safety. When records are digital, your GP and your home carer can see the same information instantly. This interoperability reduces medication errors and ensures your bespoke care plan is followed accurately.
Our priority is your safety and privacy. These systems are built with strict GDPR compliance and robust cyber security standards. The digital shift supports the NHS Long Term Plan, making the system more resilient. Key benefits of this digital integration include:
-
Real-time updates: Carers can log changes in health immediately, allowing for faster medical intervention.
-
Reduced admin: Staff spend less time on paperwork and more time providing compassionate, person-centered care.
-
Better coordination: Information follows the individual, so no detail about your preferences or needs is lost during transitions between services.
This social care and health act ensures that the UK care system is prepared for the future. It moves us toward a model where technology and human warmth work hand in hand. We believe these changes are essential for providing the high-quality, reliable support your loved ones deserve.
Navigating Compliance: Linking Legislation to CQC Standards
Compliance isn’t just a matter of following rules; it’s about the safety and dignity of the people we support. The Care Quality Commission (CQC) uses five key domains to judge how well a provider adheres to the social care and health act. These domains-Safe, Effective, Caring, Responsive, and Well-led-act as a bridge between high-level legislation and daily care delivery. When you understand how the law dictates these standards, you can provide better, more consistent support for your loved ones.
The regulatory landscape is shifting toward the Single Assessment Framework, which will be fully embedded by 2026. This new approach moves away from one-off inspections and focuses on continuous monitoring. You’re now legally required to maintain robust auditing and quality assurance systems. Proving compliance requires a clear trail of evidence that shows you’re meeting every legal mandate. Digital tools have become essential here, as they allow providers to pull real-time reports that demonstrate safety and effectiveness during any CQC check.
Evidence-Based Compliance
We believe that high-quality care must be backed by hard data. To meet clinical safety mandates, providers often use specific tools like waterlow assessment scores to manage pressure ulcer risks. This isn’t just paperwork; it’s a legal requirement to ensure the "Safe" domain is met. Similarly, the score must plays a vital role in meeting nutritional standards under the social care and health act. By using these tools, we create a "Golden Thread" of evidence. This thread connects your overarching care policies directly to the specific, bedside actions taken by staff, ensuring nothing is left to chance.
Avoiding Legal Pitfalls
Many care providers run into trouble when their documentation doesn’t reflect the care they actually provide. One of the most common legal pitfalls is relying on outdated paper records. In a digital-first environment, paper systems are often too slow to react to legislative changes. If a policy is updated in Westminster, a paper-based home might take weeks to catch up, leaving them vulnerable during an inspection. Using a digital policy library ensures that your team always has access to the most current guidance. It removes the guesswork and provides the peace of mind that your service remains on the right side of the law.
If you need help navigating these complex regulations, we’re here to guide you. Contact our expert team for bespoke care advice today.
Future-Proofing Your Care Service: A Digital Roadmap
The social care and health act of 2022 represents a fundamental shift toward integration, making digital transformation the only logical path forward for modern providers. It’s no longer just about staying current; it’s about creating a foundation where information flows freely between services to protect the person at the centre of care. We believe that moving to a digital model shouldn’t feel like a cold, technical hurdle. Instead, it’s a way to reclaim the human element of your service by removing the administrative friction that leads to burnout and oversight.
A bespoke digital approach allows you to tailor your management systems to the specific needs of your clients. This isn’t a one-size-fits-all solution. It’s a precise tool that ensures every "dedicated professional" on your team has the exact insights they need to maintain a client’s independence and dignity. When your systems are aligned with the social care and health act, compliance stops being a periodic stress and becomes a quiet, constant reassurance that your service is operating at the highest possible standard.
Embracing Digital Care Planning
Digital care planning is the bridge between clinical excellence and genuine human warmth. By streamlining your documentation, you allow your staff more time for "compassionate care" rather than tethering them to clipboards and filing cabinets. The Department of Health and Social Care has set a clear expectation for 80% of CQC-registered providers to adopt digital social care records by March 2026. Meeting this goal early ensures you have immediate data access, which is essential for real-time monitoring and responding to the changing needs of those you support.
-
Reducing Human Error: Automated medication alerts and digital incident logs significantly lower the risk of missed doses or overlooked trends.
-
Real-Time Transparency: Immediate access to care notes provides families with the "peace of mind" they deserve, knowing their loved one’s sanctuary is being monitored with precision.
-
Standardised Safety: Digital systems ensure that every entry meets the rigorous standards required for modern UK inspections.
The Care Daily Advantage
We’ve designed our platform to act as your "Trusted Local Expert," taking the guesswork out of complex legislation. Our library of 2,000+ policies is meticulously mapped to the latest UK health and care regulations, ensuring your documentation is always professional and up to date. We don’t just provide a system; we provide a partnership that prioritises the quality of life for your clients and the operational safety of your business.
Our bespoke support helps you transition from viewing compliance as a burden to seeing it as a competitive benefit. We invite you to join us for a consultation to discuss how we can bring total compliance and "peace of mind" to your operations. It’s time to move toward a future where your care service is as resilient as it is compassionate. Contact us today to begin your digital transition and secure the continuity of care your families rely on.
Securing the Future of Your Care Service
Navigating the complexities of the social care and health act requires more than just awareness; it demands a proactive approach to integration. By 2026, every UK provider must align their operations with the Integrated Care Systems established under the Health and Care Act 2022. You’ve seen how the shift from the 2012 competition model to today’s collaborative framework impacts your daily CQC compliance. Transitioning to digital care planning isn’t just a recommendation anymore. It’s a necessity for meeting the CQC’s Single Assessment Framework standards. We understand that keeping up with these shifts can feel like a heavy burden on your team. That’s why we’ve built tools to help you maintain excellence without the stress.
Our CQC-compliant policy library is fully updated for 2026 legislation to give you total peace of mind. We provide bespoke implementation and training so your staff feel confident using our digital care planning platform. You don’t have to face these regulatory changes alone. Ensure your agency is 100% compliant with the latest Social Care and Health Acts with Care Daily . We’re here to help you protect the dignity and independence of those you support every single day.
Frequently Asked Questions
What is the main difference between the 2012 and 2022 Health and Care Acts?
The 2012 Act focused on competition and market-led services, while the 2022 Health and Care Act prioritizes integration and collaboration. You’ll find that the 2022 legislation officially established 42 Integrated Care Systems across England to join up NHS and local authority services. It moves away from the previous internal market system to ensure your loved one receives more seamless support between hospital and home.
Is it a legal requirement for UK care providers to use digital records in 2026?
It’s a clear government target rather than a standalone criminal law, but the Department of Health and Social Care aims for 80% of CQC registered providers to have digital social care records by March 2024. By 2026, these digital standards will likely be a core requirement for maintaining your registration and demonstrating safe care. We recommend transitioning now to ensure you’re compliant with the Digitising Social Care programme’s expectations.
How does the Social Care and Health Act affect CQC inspections?
The social care and health act grants the CQC new powers to review and rate how local authorities deliver their care duties under the Care Act 2014. This means inspectors don’t just look at individual care homes; they now assess how the entire local system supports residents. You’ll see a greater focus on how different services work together to maintain your independence and safety during future inspections.
What are Integrated Care Systems (ICS) and why do they matter to care homes?
Integrated Care Systems are 42 regional partnerships that bring together NHS providers, local councils, and care home managers to plan health and care services collectively. For care homes, this matters because it simplifies the way you access specialist medical support for your residents. It’s designed to reduce hospital admissions by ensuring a GP or district nurse is more involved in the bespoke care plans we create for our clients.
Does the Health and Social Care Act apply to domiciliary care agencies?
Yes, the 2022 Act applies directly to domiciliary care agencies as they’re a vital part of the broader social care landscape. The legislation ensures that home-based support is integrated into the wider healthcare network, giving you peace of mind that your home care provider is connected to your NHS records. This helps maintain your dignity and independence by ensuring every professional involved in your care is on the same page.
How often should care policies be updated to reflect new legislation?
You should review your care policies at least once every 12 months, or immediately when new legislation like the 2022 Act introduces specific changes. Staying current ensures your team follows the latest safety protocols and legal requirements. We suggest setting a fixed date for an annual audit to keep your bespoke care standards aligned with the social care and health act and CQC expectations.
What is the "Duty of Candour" in the context of health and social care law?
The Duty of Candour is a legal requirement under Regulation 20 of the 2014 Regulations for care providers to be open and honest with families when something goes wrong. If an incident occurs that results in moderate or severe harm, we must notify you as soon as possible, provide a truthful account, and offer a formal apology. This regulation ensures transparency and builds the trust you need when choosing a partner for your loved one’s care.
Can I still use paper-based care plans under the 2022 Act?
You can still use paper-based plans for now, but the 2022 Act makes it much harder to meet the evolving standards for data sharing and safety. The government’s "Data Saves Lives" strategy targets a move away from paper to ensure information follows the person. Switching to digital bespoke care plans helps prevent errors and ensures that emergency services have instant access to vital health details if they’re ever needed.