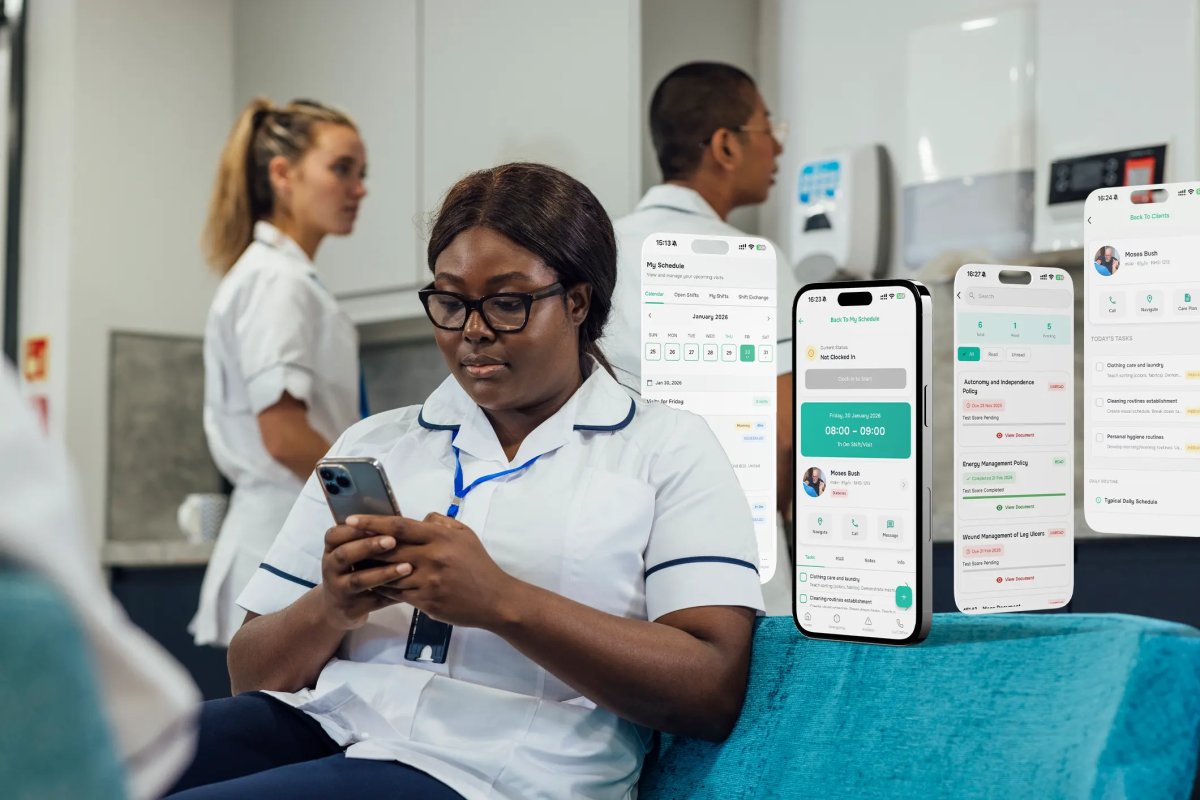
Did you know that treating pressure ulcers costs the NHS more than £3.8 million every single day? For a dedicated care provider, these figures represent more than just a financial burden; they reflect a person’s lost comfort and independence. Accurately calculating a waterlow assessment score is your first line of defence in protecting those you care for from avoidable harm. It’s the difference between a proactive care plan and a reactive crisis that could lead to a "Requires Improvement" rating from the CQC.
You likely feel the weight of responsibility when documenting risk, especially when staff members interpret mobility or nutrition factors differently. We understand that you want your team to feel confident and your records to be audit-ready at a moment’s notice. This guide helps you master the Waterlow system to ensure every service user receives bespoke support for their skin integrity. You’ll learn how to navigate the complexities of the scoring tool, simplify your documentation process, and provide the peace of mind that comes with exceptional, person-centred care.
Key Takeaways
-
Learn how to identify early signs of risk and protect your service users’ dignity by mastering the foundational principles of pressure ulcer prevention.
-
Master the seven key risk factors to accurately calculate a waterlow assessment score, ensuring every individual receives a bespoke care plan tailored to their specific needs.
-
Understand the distinct advantages of using the Waterlow scale over the Braden tool to maintain the high standards of safety expected within the UK social care sector.
-
Discover how regular re-assessments support CQC compliance, helping you demonstrate "Safe" and "Effective" care delivery during your next inspection.
-
See how transitioning to digital care planning provides real-time alerts and peace of mind, ensuring your team can respond swiftly to protect the health of those in your care.
Table of Contents
What is the Waterlow Assessment Score in UK Care?
Pressure ulcers can cause significant physical distress and reduce a person’s quality of life. We believe every individual deserves to live without the pain of preventable skin breakdown. The waterlow assessment score is a vital tool used by healthcare professionals across the UK to identify those at risk and prevent these injuries before they start. It provides a structured framework that helps our dedicated professionals deliver the highest standard of support.
Developed by Judy Waterlow in 1985 while she was working as a Clinical Nurse Teacher, this tool was designed specifically for the UK healthcare landscape. It’s now one of the most frequently used methods for assessing pressure sore risk in hospitals, nursing homes, and home care settings. Understanding What is the Waterlow Score? involves looking at various physical and lifestyle factors to create a bespoke prevention plan for each person.
Protecting skin integrity is a cornerstone of person centred care. When we focus on the whole person, we ensure their dignity and independence remain intact. Whether your loved one is in a residential facility or receives domiciliary care at home, this assessment offers peace of mind. It ensures that their physical health is monitored with expert precision and genuine compassion.
The Core Purpose of Pressure Ulcer Risk Assessment
The primary goal is proactive prevention. By identifying vulnerable service users early, we can implement support like specialist mattresses or specific repositioning schedules. Establishing a baseline for skin integrity during the initial care intake ensures we notice even the smallest changes over time. This tool also provides a standardised language. It allows our team to communicate clearly with GPs, district nurses, and multidisciplinary teams, ensuring total continuity of care.
Who is Responsible for Conducting the Assessment?
Registered Nurses usually lead these evaluations in clinical or nursing home settings. However, trained senior care assistants often perform the waterlow assessment score in residential or home-based environments. It’s essential that any staff member using clinical tools meets strict competency requirements. We don’t just rely on the numbers. Professional judgement remains crucial. While a score provides the data, the insight of a compassionate guide ensures the final care plan truly reflects the individual’s unique needs and lifestyle.
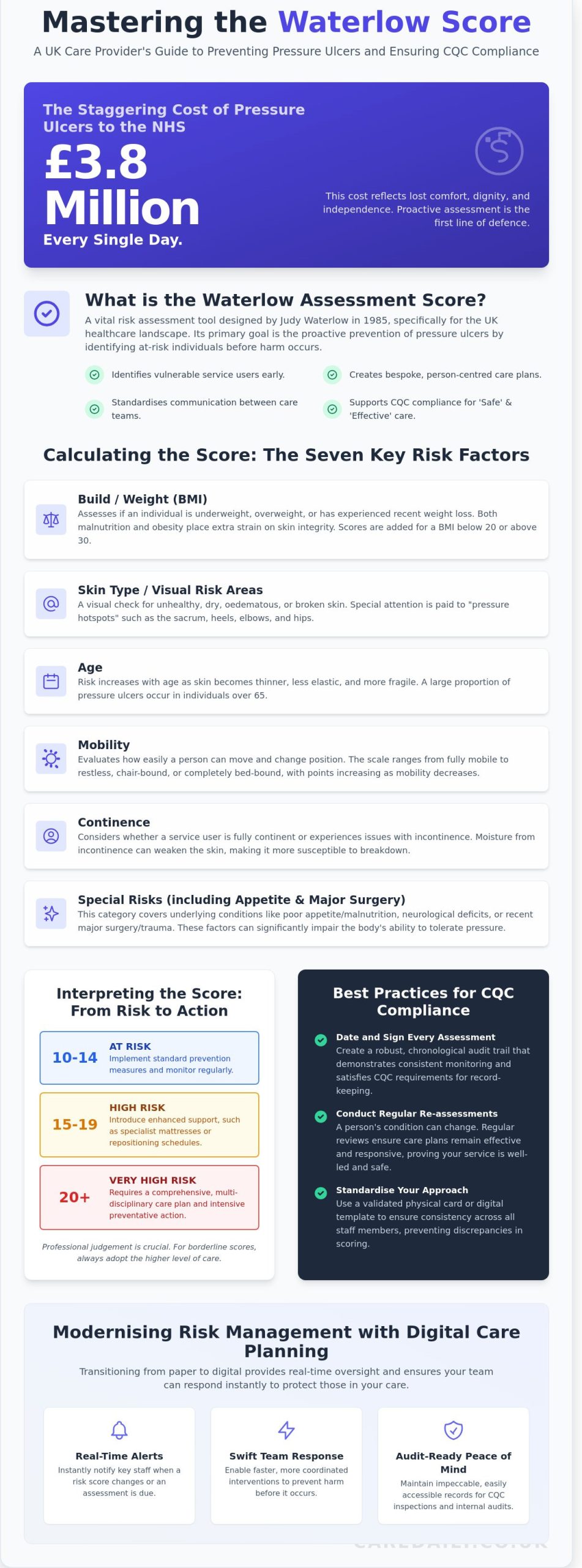
Calculating the Waterlow Score: The Seven Key Risk Factors
You calculate the waterlow assessment score by adding points across seven distinct clinical categories. This cumulative system ensures that no single factor is overlooked when evaluating a person’s vulnerability. A total score of 10 to 14 indicates the individual is "at risk," 15 to 19 signifies "high risk," and any score of 20 or above represents "very high risk." You should use a physical Waterlow card or a validated digital template to ensure your results remain consistent across the entire care team. This standardisation prevents discrepancies between different staff members.
Clinical expertise is vital during this process. If a service user sits on a borderline score, your professional judgement ensures they receive the higher level of preventative care they need. We recommend that every assessment you complete is dated and signed immediately. This creates a robust audit trail that satisfies CQC requirements and provides a clear history of the person’s skin health journey. It’s about more than just a number; it’s about creating a reliable record of safety.
Breakdown of the Primary Clinical Factors
You begin by assessing the individual’s build and weight. A Body Mass Index (BMI) that falls below 20 or rises above 30 adds points to the score, as both malnutrition and obesity put extra strain on skin integrity. You will also perform a visual skin assessment, paying close attention to "pressure hotspots" like the heels and sacrum. Age is a significant factor in the waterlow assessment score too. Statistics from the NHS indicate that a large proportion of pressure ulcers occur in people over the age of 65. Because skin becomes thinner and less elastic with age, older service users require more frequent monitoring to stay safe.
Analysing Mobility and Continence
Your assessment looks at how easily a person moves. The scale ranges from "fully mobile" to "restless," "chair-bound," or "bed-bound." Higher points are assigned to those with limited movement because prolonged pressure restricts blood flow to the tissues. Continence is equally critical. Constant moisture can lead to skin maceration, which makes the tissue much more likely to break down. While total incontinence carries a high risk score, you will adjust this for service users using catheters. These devices help manage moisture levels and reduce direct skin contact with irritants, which can lower the immediate risk to the skin.
Evaluating Nutrition and Special Risks
We know that poor nutrition directly impacts how the body maintains its natural barriers. A lack of protein or vitamins leads to delayed healing and fragile tissue. You must also consider special risks such as neurological deficits, which might prevent a person from feeling the discomfort of a developing sore. Medication is another key factor. If a resident takes high-dose steroids or anti-inflammatories, their skin becomes significantly thinner and more prone to tearing. Ensuring that a resident’s MUST score must be accurately recorded alongside their Waterlow assessment gives your team a complete picture of their nutritional vulnerability and skin integrity risk. Our bespoke care planning helps you integrate these findings into a daily routine that prioritises comfort and dignity for every individual.
Waterlow vs. Braden: Choosing the Right Tool for Your Service
Selecting the right risk assessment tool is a vital step in providing bespoke care that truly protects your residents. While the Braden Scale is widely used globally, the waterlow assessment score remains the most prevalent choice across the UK social care landscape. We understand that you want to ensure your team uses the most effective method to maintain the dignity and physical health of those in your care. Choosing a tool that fits your specific environment provides your staff with the confidence they need to deliver excellent support.
The primary difference between these two systems lies in the level of detail regarding physiological factors. The Braden Scale focuses heavily on sensory perception and moisture, which is often ideal for acute hospital settings. In contrast, Waterlow incorporates a broader range of "special risks" such as specific medications, neurological deficits, and the nuances of the ageing process. We recommend maintaining clinical consistency by sticking to one tool. Switching between different scales, often called "tool hopping," can lead to fragmented data. This makes it difficult for your dedicated professionals to track a resident’s progress or identify a subtle decline in skin integrity.
When to Use the Waterlow Scale
We find that the Waterlow Scale is particularly suited for elderly populations within UK care homes. It offers a comprehensive view of a person’s health by considering factors that other scales might overlook. It’s the preferred choice for several reasons:
-
Clinical Depth: It accounts for the impact of certain surgeries and long-term medication use.
-
Standardisation: Most NHS trusts and local authorities in England and Wales use this scoring system as their primary language for reporting.
-
Continuity of Care: Using the same system as local hospitals ensures a seamless transition for residents, providing much-needed peace of mind for families.
Limitations and When to Seek Specialist Advice
Your clinical judgement is the most powerful tool you have. A waterlow assessment score provides a structured guide, but it’s not a final diagnosis. One common challenge is "over-scoring," where a resident is marked as higher risk than they truly are. This can sometimes lead to unnecessary clinical interventions that might inadvertently limit a resident’s independence. We always encourage our partners to view the score as one part of a holistic, person-centered plan.
Safety must always be the priority. If a resident reaches a score of 20 or higher, they are categorised in the "very high risk" group. In these instances, you should make an immediate referral to a Tissue Viability Nurse (TVN). Our goal is always to provide proactive support before a pressure ulcer can develop, ensuring every individual enjoys the highest possible quality of life in their own home environment. This collaborative approach between your team and specialist nurses builds a robust safety net for those you support.
Implementing Waterlow Assessments for CQC Compliance
We know that your priority is the safety and comfort of those you support. The Care Quality Commission (CQC) shares this focus, specifically through their "Safe" and "Effective" key lines of enquiry. A consistently updated waterlow assessment score provides the objective evidence inspectors look for to prove you are proactively managing skin integrity. When you link these scores to your incident and accident reporting, you create a transparent audit trail. This shows that you don’t just record risks; you respond to them with compassion and clinical precision.
Your assessment data also serves as a vital business tool. If a service user’s score indicates a high risk, you have the clinical justification needed to invest in specialist pressure-relieving equipment. Whether it is a £400 foam mattress or a £2,000 dynamic airflow system, the Waterlow score ensures your spending is targeted where it will most improve a person’s quality of life. It transforms a request for funding into a professional, evidence-based requirement. Staying current with the social care and health act framework ensures your funding decisions and care protocols align with the latest legislative standards.
Frequency of Re-assessment and Review
You should establish a regular rhythm for reviews to maintain peace of mind for both staff and families. For those at low risk, a monthly review is often sufficient. However, for individuals with a high waterlow assessment score, we recommend weekly checks. You must also trigger an immediate re-assessment following "change of state" events. These include hospital discharges, bouts of illness, or significant weight changes. Documenting these triggers shows the CQC that your care is bespoke and responsive rather than a routine exercise.
Avoiding Common Errors in Scoring
One of the most frequent pitfalls during inspections is the "copy and paste" trap. If every monthly assessment looks identical, it suggests the carer hasn’t truly observed the individual’s skin or mobility. You should ensure that mobility and nutrition categories reflect the person’s current reality, not just their history. To eliminate human error, many providers now use digital care management software UK . These systems calculate scores automatically, ensuring accuracy and freeing your team to spend more time on meaningful companionship.
Our dedicated professionals are here to help you manage the complexities of CQC compliance with confidence. Contact CareDaily today to learn how we support your commitment to excellence.
Modernising Risk Management with Digital Care Planning
We understand that the traditional paper-based Waterlow card has been a staple in UK care settings for decades. However, the shift towards digital social care records, backed by the Department of Health and Social Care’s target for 80% of CQC-registered providers to have digital records by March 2024, has changed the landscape. Moving your risk management online isn’t just about efficiency; it’s about dignity. When you digitise the waterlow assessment score, you ensure that every vulnerable person receives the precise level of protection they deserve without the delays of manual filing.
Our dedicated professionals use these tools to provide a "calm in the storm" experience for families. Digital systems offer real-time alerts. If a service user’s score increases to a high-risk threshold of 15 or above, the system notifies managers instantly. This proactive approach prevents small concerns from becoming serious medical issues, giving you and your family total peace of mind. By positioning your agency as a tech-forward provider, you demonstrate that you prioritise the safety of those in your care above all else.
Benefits of Electronic Waterlow Assessments
Manual calculations are often prone to human error; industry data suggests that up to 20% of paper-based clinical scores may be calculated incorrectly. Digital assessments eliminate this risk by automating the mathematics. We ensure that no risk factor is overlooked through mandatory data fields, meaning an assessment cannot be finished until every skin health indicator is recorded. Managers can view these scores across multiple sites via a single dashboard, providing a level of oversight that paper folders simply cannot match.
From Scores to Actionable Care Plans
A numerical waterlow assessment score is only useful if it leads to direct action. Digital platforms bridge this gap by suggesting bespoke interventions the moment a score is saved. If a person is identified as "At Risk," the system can automatically generate a repositioning schedule or "turning chart" for our care teams to follow. This creates a robust, timestamped audit trail that proves high-quality care was delivered and helps you remain compliant with CQC Regulation 12 regarding safe care and treatment.
We also use digital portals to share this vital data with GPs and district nurses instantly. This collaborative approach means that if a skin integrity issue arises, the wider multi-disciplinary team has the facts they need to respond. You aren’t just filing a report; you’re building a protective circle around your loved one’s independence and health. This seamless flow of information ensures continuity of care, making the transition between home and clinical settings much safer for everyone involved.
Prioritising Resident Safety Through Digital Innovation
Protecting your residents from the risk of pressure ulcers starts with a robust waterlow assessment score. It’s more than just a clinical metric; it’s a foundation for maintaining dignity and independence in every UK care setting. By moving away from paper-heavy processes and embracing bespoke digital tools, your team can focus on what matters most: the person. Ensuring CQC compliance doesn’t have to be a burden when you have the right systems in place. We’ve developed over 2,000 CQC-compliant policies and procedures to give you total peace of mind that your service meets every regulatory standard. These bespoke digital care planning tools are trusted by providers across the country to support continuity of care, helping your dedicated professionals provide the high-quality support your residents deserve. Your residents deserve the best. You can transform your risk management into a seamless, compassionate process that puts safety first. Discover how Care Daily simplifies CQC compliance with digital risk assessments and start your journey towards a more secure, person-centred future today.
Frequently Asked Questions
What is a "good" Waterlow score?
A lower score is better because it indicates a lower risk of your loved one developing pressure sores. A score below 10 is considered low risk, meaning their skin is currently healthy and resilient. If the waterlow assessment score reaches 15 or higher, it signals a high risk that requires us to introduce specialised equipment and bespoke care plans to maintain their comfort.
How often should a Waterlow assessment be updated?
You should update the assessment at least every 30 days in a stable home environment or weekly in a clinical setting. Our dedicated professionals recommend a new assessment immediately if a person’s health changes, such as after a hospital stay or a fall. This ensures their support remains accurate and provides you with essential peace of mind about their safety.
Is the Waterlow score mandatory for CQC compliance?
The CQC doesn’t mandate the Waterlow tool specifically, but Regulation 12 requires all UK providers to manage skin integrity risks effectively. Approximately 90% of care providers use recognised tools like Waterlow or Braden to demonstrate they’re meeting these safety standards. Using this established system helps us provide a high level of clinical competence while honouring the dignity of those we support.
Can a care assistant complete a Waterlow assessment?
A trained care assistant can complete the assessment if they’ve been officially signed off as competent by their manager. In most UK settings, a registered nurse or a senior lead will then review the final waterlow assessment score to ensure its accuracy. This collaborative approach ensures that the daily observations of our companions are backed by expert clinical oversight.
What is the difference between Waterlow and the MUST score?
The Waterlow tool measures the risk of pressure ulcers, while the Malnutrition Universal Screening Tool (MUST) score identifies if someone is at risk of being underweight or malnourished. While they’re different, they often work together since a high MUST score can increase a person’s Waterlow risk. We use both to create a holistic view of health that protects a person’s independence.
What happens if a service user refuses a skin inspection for the assessment?
We always respect a person’s right to refuse an inspection, as maintaining their privacy and agency is our primary goal. If your loved one declines, we’ll document the refusal clearly and use other factors like mobility and diet to estimate their risk level. Our team then works as a compassionate guide to find alternative ways to keep their skin healthy without causing distress.
Is the Waterlow assessment free to use for care providers?
The Waterlow score is free for all care providers to use because it’s in the public domain. Judy Waterlow designed the tool in 1985 to ensure that all healthcare professionals could access a reliable way to prevent pressure sores. This allows us to focus our resources on providing high-quality, personalised care rather than paying for expensive software licences.
What should I do if a service user’s score increases suddenly?
If a score increases by 2 points or more, you should immediately review the care plan and consult a GP or tissue viability nurse. A sudden rise often means the person needs new pressure-relieving cushions or a change in their repositioning schedule. We act quickly in these moments to ensure their home remains a safe sanctuary and to prevent any further health complications.