What if the 15 minute care window wasn’t a barrier to dignity, but the foundation for a life lived with purpose? You likely agree that the relentless pressure of the clock often forces your dedicated professionals to focus on checklists rather than the human being in front of them. It’s a common struggle for UK providers who feel the weight of the CQC’s “Caring” domain while trying to manage person centred care in a high-pressure environment. You want your team to provide more than just a service; you want them to provide a sanctuary where independence is preserved at all costs.
This guide shows you how to transform your delivery, ensuring you don’t just meet the CQC’s 2026 Quality Statements but actually exceed them. We’ll help you move away from task-led routines and towards personalised, bespoke support that protects a service user’s peace of mind. You’ll gain a clear understanding of core principles alongside practical daily strategies and documentation frameworks that prove your commitment to quality of life. We’ve designed this to give you the confidence to lead your team through the latest regulatory shifts with ease, expertise, and genuine warmth.
Key Takeaways
- Learn how to transition from a clinical ‘medical model’ to a social model that prioritises a resident’s life and identity beyond their diagnosis.
- Discover the four core pillars of person centred care and how embracing positive risk-taking can safely enhance a person’s independence and dignity.
- Uncover practical strategies to overcome time constraints and staff turnover, ensuring your team maintains a consistent and calm environment for those they support.
- Master the art of creating bespoke care plans that move beyond generic tick-boxes to capture the unique ‘who’ behind every individual.
- See how integrating digital tools and compliant policy libraries can reduce administrative burdens, giving your staff more time for meaningful human connection.
Understanding Person-Centred Care: More Than Just a Buzzword
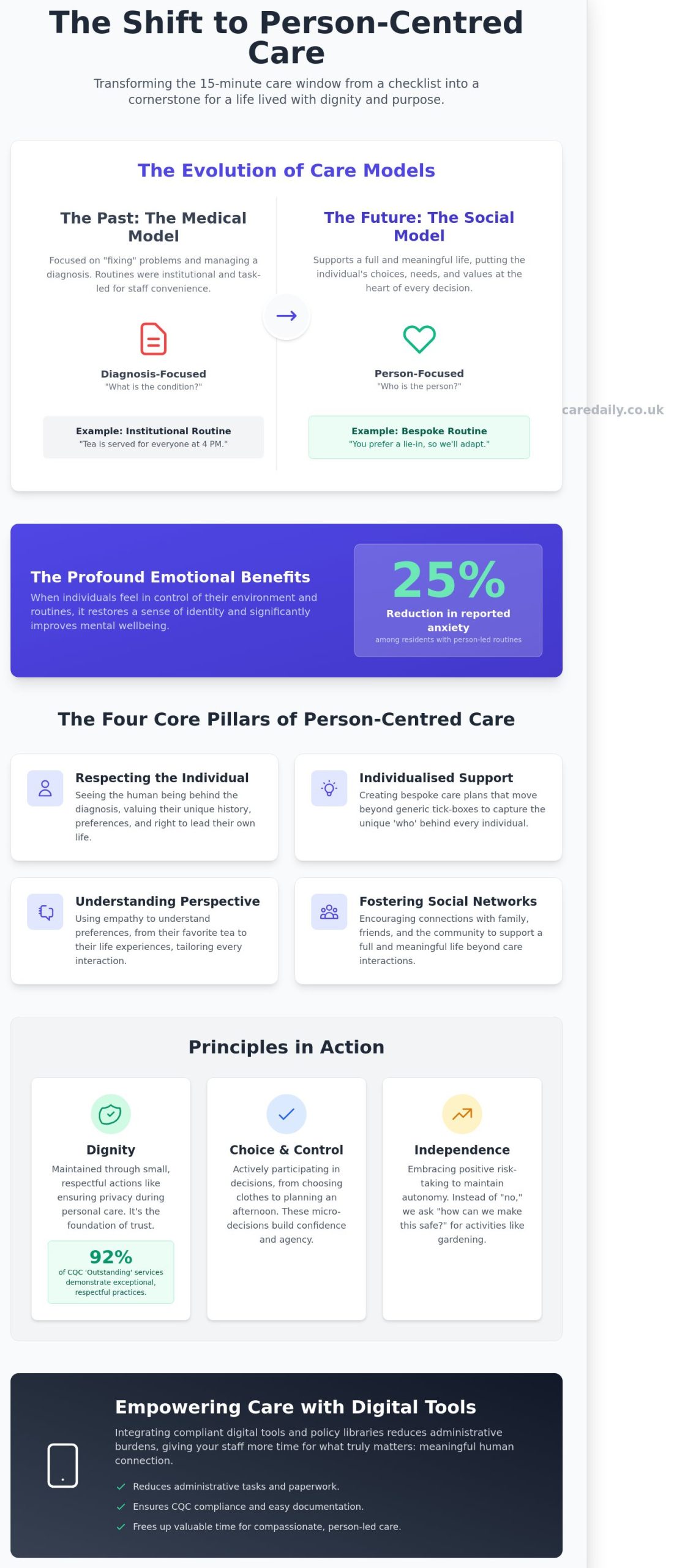
You want your loved one to feel seen, heard, and valued, not just managed like a set of symptoms. Person centred care is the practice of putting the individual’s choices, needs, and values at the heart of every care decision. It moves us away from the outdated medical model, which historically focused on “fixing” physical problems or managing a diagnosis. Instead, we embrace the social model, which focuses on supporting a full and meaningful life regardless of health challenges.
This shift represents a fundamental change in how we view support. We no longer see a “dementia patient” or a “mobility case”; we see a person with a unique history, a specific set of preferences, and a right to lead their own life. In 2026, this approach is the foundational expectation for the Care Quality Commission (CQC) and is enshrined within the Health and Social Care Act. It ensures that every interaction provides dignity and peace of mind for both the individual and their family.
The Evolution of Care: From Task-Led to Person-Led
In the past, many UK care settings followed an institutional approach. Routines dictated the person’s day, often for the convenience of the staff or the building’s schedule. If tea was served at 4 pm, everyone drank tea at 4 pm. Modern person-led care completely flips this script. Now, the person dictates the routine. If they prefer a lie-in until 10 am and a light supper at midnight, the care plan adapts to them.
The emotional benefits of this agency are profound. When service users feel in control of their environment, we see significant improvements in mental health. Data from UK care providers suggests that bespoke, person-led routines can lead to a 25% reduction in reported anxiety levels among residents. It restores a sense of identity that rigid, task-led systems often strip away.
The Legal and Regulatory Framework in the UK
The legal landscape in England and Wales firmly supports this human-first approach. The Care Act 2014 established “wellbeing” as the primary duty for all local authorities and care providers. This means your care isn’t just about safety; it’s about your overall quality of life. The CQC reflects this in their inspection framework, where the “Caring” and “Responsive” domains specifically hunt for evidence that a provider treats people as individuals.
To meet these high standards, providers must demonstrate that they listen to and act upon the wishes of those they support. Maintaining these records is vital for staying on the right side of the law. For more details on how technology helps meet these 2026 standards, you can view our Digital Care Management Software UK guide. Staying compliant ensures that your service remains a safe, compassionate sanctuary for every individual in your care.
The Core Principles: Dignity, Choice, and Independence
We believe that high-quality care isn’t just about ticking boxes on a medical chart. It’s about seeing the human being behind the diagnosis. To deliver true person centred care, we rely on four fundamental pillars: respecting the individual, providing individualised support, understanding the person’s unique perspective, and fostering a strong social network. These pillars ensure that every interaction is grounded in respect rather than routine.
Empathy is our bridge to understanding. When we know that a client prefers Earl Grey tea at 4:00 PM or that they spent 35 years as a primary school teacher, we can tailor our approach to suit their soul. This isn’t just a “nice to have” feature; it’s essential for emotional well-being. Dignity is maintained through the smallest, most quiet actions. During personal care, our companions ensure doors are closed and towels are used to maintain modesty, protecting the privacy of every individual we support. A 2023 report from the Care Quality Commission (CQC) found that 92% of services rated “Outstanding” demonstrated these exceptional, respectful practices.
Promoting Choice and Control
You deserve to lead your own life, regardless of your care needs. We encourage active participation, which means doing things with you, rather than to you. Whether it’s choosing a blue jumper or deciding how to spend a sunny Tuesday afternoon, these micro-decisions build confidence. We also embrace positive risk-taking. If a client wants to continue light gardening despite mobility issues, we don’t just say “no.” Instead, we find ways to make it safe, perhaps by using raised beds or specialised tools. This approach respects your autonomy while maintaining safety.
Valuing the Individual’s Unique History
Our dedicated professionals use ‘Life Story’ work to connect with those living with dementia or age-related frailty. By documenting your cultural background, religious beliefs, and past hobbies, we can manage challenging behaviours with genuine compassion. If a client becomes distressed, knowing their favourite 1940s swing record can often provide instant comfort. We ensure every bespoke care plan reflects these personal details, honouring the life you’ve lived. If you’re looking for this level of detail, you can explore our bespoke care options to find the right fit for your family. This commitment to person centred care ensures that your history is never forgotten, but used to brighten your present.
Common Barriers to Personalised Care (and How to Overcome Them)
Implementing person centred care often feels like an uphill struggle against systemic pressures. You might feel that your team is constantly “firefighting” rather than providing bespoke support. A 2024 report by Skills for Care highlighted that the adult social care sector still faces a 28.3% staff turnover rate. This churn makes maintaining a “continuity of care” difficult, as new staff struggle to learn the nuances of a resident’s life history quickly. When faces change every week, the deep trust required for genuine support is harder to build.
Institutional mindsets often persist because of outdated, paper-based systems. These folders frequently hide the individual behind a wall of clinical jargon and rigid schedules. When care is dictated by a clipboard rather than a conversation, dignity is often the first thing lost. We see this when well-meaning teams prioritise task completion over human connection. Breaking these habits requires a shift in focus from “what is the matter with you” to “what matters to you.”
Dispelling the ‘Time Constraint’ Myth
The most common objection we hear is that there isn’t enough time. However, investing time to understand a resident’s specific behaviour triggers actually prevents escalating crises. Research suggests that proactive engagement can reduce incidents of distress by up to 30%. By knowing that a certain song or a specific morning routine provides peace of mind, your team avoids the time-consuming fallout of a distressed resident. Ultimately, person-centred care is not an ‘add-on’ time-consumer, but a more efficient way to deliver support.
Addressing the Training Gap
We must move away from “tick-box” training that focuses solely on compliance. Real change happens through values-based induction. You should empower junior staff to make small, person-centred decisions without fearing they are “breaking the rules.” If a resident wants breakfast at 10:00 am instead of 8:00 am, the system should flex to accommodate them. Leadership plays a vital role here by modelling empathetic behaviour for the whole team. When managers demonstrate that they value independence over rigid adherence to a schedule, the whole team follows suit. This shift creates a sanctuary where residents feel truly at home.
- Digital Transition: Move away from paper to surface the “person” behind the paperwork.
- Empowerment: Allow staff to deviate from routines if it benefits the resident’s wellbeing.
- Consistency: Prioritise stable rotas to ensure person centred care remains the standard.
By addressing these barriers head-on, you transform your service from a clinical facility into a true home. It’s about creating a culture where every interaction is an opportunity to reinforce a person’s identity and autonomy. Effective staff rostering in social care ensures that the same familiar faces provide consistent support, building the trust necessary for meaningful person-centred relationships.
Practical Steps to Implementing Person-Centred Care Plans
We believe that a care plan shouldn’t be a static document hidden in a filing cabinet. It’s a living roadmap. In 2026, 85% of CQC-rated “Outstanding” providers have moved away from “one size fits all” assessments to bespoke planning. This shift captures the “who” behind the person, rather than just the “what” of their medical condition. You need to establish a cycle of constant review where the person’s voice remains the loudest. This ensures that dignity and independence stay at the heart of every interaction.
Creating a Digital Care Plan That Truly Reflects the Individual
Modern digital care planning allows us to store rich media that brings a person’s history to life. Instead of a clinical note saying “needs assistance with washing”, we record that a client “prefers a bath at 8 am with lavender oil”. We use photos of family pets and videos of preferred morning routines to guide staff. This level of detail ensures that every carer on shift, whether they’ve known the client for years or just a day, provides consistent, compassionate support. Daily notes now focus on person centred care outcomes, such as how a resident felt during an activity, rather than just ticking a task list.
Involving the Circle of Support
We treat families and advocates as partners, not just observers. Our family portals provide 24/7 access to updates, which helps reduce the anxiety often felt by loved ones. For those with limited capacity or no local family, we work closely with independent advocacy services to ensure their rights are protected. This collaborative approach builds a bridge of trust and provides peace of mind for everyone involved.
Co-producing care goals means the service user decides what success looks like. Whether it’s walking to the local park or maintaining a specific hobby, these goals are meaningful because they’re chosen by the individual. By integrating person centred care into every daily interaction, we help people maintain their identity. We use technology to make this personalised information instantly accessible to every carer on shift, ensuring no detail is missed.
Speak with our compassionate team today to discover how we can build a bespoke care plan for your loved one.
How Care Daily Empowers Your Person-Centred Journey
We understand that the heart of your service isn’t a spreadsheet or a filing cabinet. It’s the quiet moment a carer spends listening to a resident’s life story over a cup of tea. However, the administrative weight of 2026 compliance requirements can often bury those moments under a mountain of paperwork. Care Daily acts as your silent partner. We manage the complex regulatory framework so your team can return to what they do best: providing bespoke, compassionate support.
Our platform is built on the belief that technology should never replace human connection. Instead, it should facilitate it. By automating routine administrative tasks, we’ve seen providers reclaim up to 12 hours of staff time per week. This time is redirected where it matters most: with the people you support. We handle the compliance details, letting you focus on the person, not the process.
Policies That Protect and Promote Dignity
Our library contains over 2,000 bespoke policies designed specifically for the UK care market. We don’t just provide generic templates. We provide a living foundation for person centred care that respects every individual’s right to choice and independence. Every document is written by industry experts to align with the latest 2026 UK legislative changes, including the most recent updates to the Health and Care Act. For comprehensive guidance on maintaining regulatory compliance, our CQC compliant care policies and procedures guide provides essential frameworks that support both quality outcomes and inspection readiness.
- Staff access best practice guidance instantly through our intuitive mobile app.
- Automatic updates ensure your organisation never falls behind changing regulations.
- Policies are written in plain English to ensure they are actionable and clear for every team member.
Evidencing Excellence for CQC Inspections
Proving your impact to the CQC is no longer about frantic paper-chasing in the days leading up to an inspection. Our digital tools create a continuous, real-time audit trail of personalised outcomes. You can generate detailed reports that map directly to specific CQC Quality Statements. This makes it simple to show exactly how you’ve prioritised resident preferences and maintained their safety.
Whether it’s a record of a specific meal choice or a documented change in a morning routine to suit a resident’s mood, the evidence is securely stored and easily retrievable. This transparency builds trust with families and regulators alike. You can explore our person-centred care management tools and policies today to see how we simplify your path to an “Outstanding” rating. We provide the peace of mind you need to lead your team with confidence and kindness.
Elevating Your Standard of Support for 2026
You have the power to transform the lives of those you support by placing their unique needs at the heart of every decision. True person centred care isn’t a box-ticking exercise; it’s a daily commitment to dignity, independence, and individual choice. By addressing common barriers like administrative fatigue and fragmented systems, your team can finally focus on providing the bespoke support every service user deserves.
We’ve built the tools to help you lead this change with confidence. Care Daily provides a CQC compliant policy library updated for 2026, ensuring your service remains ahead of regulatory requirements. Leading UK domiciliary and residential providers already use our bespoke digital care planning modules to reduce errors and improve quality of life. It’s time to move away from rigid, institutional routines and embrace a more compassionate, flexible future for your organisation.
Request a demo of Care Daily’s person-centred management platform
You don’t have to navigate these complex regulatory changes alone. We’re here to help you build a service where every individual feels truly seen, heard, and respected.
Frequently Asked Questions
What is the difference between person-centred care and individualised care?
Person-centred care differs from individualised care by focusing on your whole life rather than just your clinical needs. While individualised care might adjust a specific task to fit you, person-centred care starts with your history, values, and personal goals to shape your entire support package. This holistic approach ensures our companions aren’t just ticking a box; they’re honouring your identity and preserving your dignity at home.
Is person-centred care a legal requirement in the UK?
Yes, person-centred care is a statutory requirement under Regulation 9 of the Health and Social Care Act 2008 (Regulated Activities) Regulations 2014. The Care Quality Commission (CQC) mandates that all registered providers must ensure your care is appropriate, meets your needs, and reflects your personal preferences. Failing to meet these standards can lead to a provider receiving a “Requires Improvement” or “Inadequate” rating during an official inspection.
How does person-centred care improve safety for service users?
This approach improves safety by reducing the risk of incidents through a deep understanding of your unique triggers and daily habits. Research from the Health Foundation in 2023 links personalised support to a 15% reduction in avoidable hospital admissions. When we understand your specific mobility patterns and routines, we can create a safer environment that prevents falls and reduces distress without resorting to restrictive practices. Proper incident and accident reporting in care ensures that any safety concerns are documented and addressed promptly to maintain this protective environment.
What are the 4 core principles of person-centred care?
The four core principles involve affording people dignity, compassion, and respect; offering coordinated care; providing personalised support; and supporting people to recognise their own strengths. These pillars ensure that every interaction is a true partnership between the professional and the individual. We use these principles to ensure our bespoke care plans focus on what you can do, rather than just the things you find difficult.
How can I involve a person with dementia in person-centred care planning?
You can involve a person with dementia by using “life story” tools and non-verbal communication to capture their likes and dislikes. Even if a person can’t express their choices verbally, you can observe their reactions to certain music, foods, or environments to build a bespoke plan. We recommend using a “This is Me” document, a tool supported by the Alzheimer’s Society, to document these vital details for every dedicated professional to follow.
What happens if a person’s choices conflict with their safety?
When a person’s choice conflicts with their safety, you must follow the principles of positive risk-taking and the Mental Capacity Act 2005. You should document a formal risk assessment that weighs the person’s right to autonomy against the potential for harm. If a person chooses to walk unaided despite a risk of falling, your role is to find a middle ground that supports their independence while minimising the danger to their health.
How do I evidence person-centred care during a CQC inspection?
You can evidence person-centred care by providing the CQC with detailed care logs that focus on outcomes rather than just completed tasks. Instead of writing “assisted with washing,” your records should reflect how the person’s preferences were met, such as “Mary chose her floral dress and preferred a morning shower.” CQC inspectors look for these specific details in your records to confirm that support is truly tailored to the individual’s wishes.
Can digital software really help with person-centred care?
Digital software significantly enhances person-centred care by providing real-time updates and ensuring every professional has access to your most current preferences. Systems like CareDaily allow for instant communication between families and carers, ensuring that a change in a loved one’s mood or needs is recorded within seconds. This technology removes the lag time of paper records, meaning your bespoke support is always accurate, responsive, and reliable.






